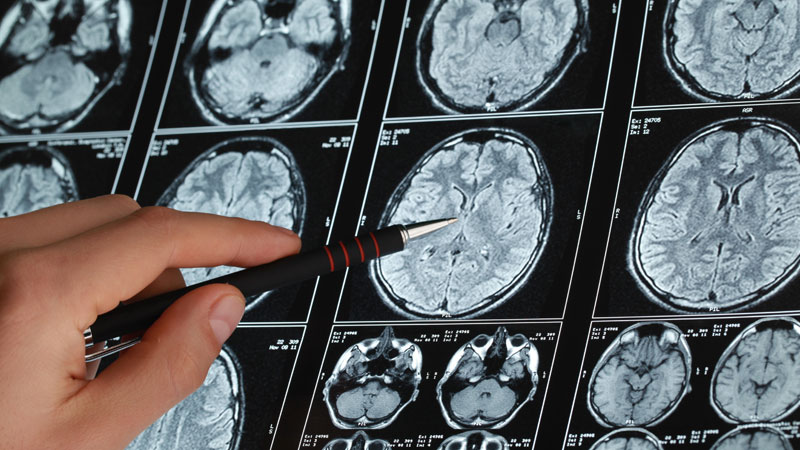
Lung cancer stands as a leading cause of cancer-related deaths globally, characterized by high mortality rates due to frequent late-stage detection, as early phases are often asymptomatic. This article offers an in-depth analysis of lung cancer, covering its development, main risk factors—such as smoking, environmental pollutants, genetic predisposition, and pre-existing lung conditions—and examining its prevalence both worldwide and within India, where rising tobacco use and pollution contribute to increasing cases. It distinguishes between the two primary types, Non-Small Cell Lung Cancer (NSCLC) and Small Cell Lung Cancer (SCLC), and describes their progression stages. The article also explores current treatment options, including surgery, chemotherapy, radiation, targeted therapy, and immunotherapy, while offering self-care strategies for patients. Emphasizing prevention, early detection, and lifestyle adjustments, the piece encourages proactive risk management to mitigate the global impact of lung cancer and improve patient outcomes.